Dental implants have become one of the safest, most effective, and long-lasting solutions for replacing missing teeth. Thanks to advances in dentistry, they currently offer success rates above 90–95%, making them a highly predictable treatment option.
However, like any medical procedure, there are risks associated with dental implants that are important to understand. Knowing these risks does not mean distrust—on the contrary, it allows you to make informed decisions and understand how they can be minimized through accurate diagnosis, careful planning, and high-quality treatment.
In this article, we clearly and thoroughly explain these risks, why they occur, and what can be done to prevent them.
What Are Dental Implants and What Do Risks Involve?
Definition of a Dental Implant
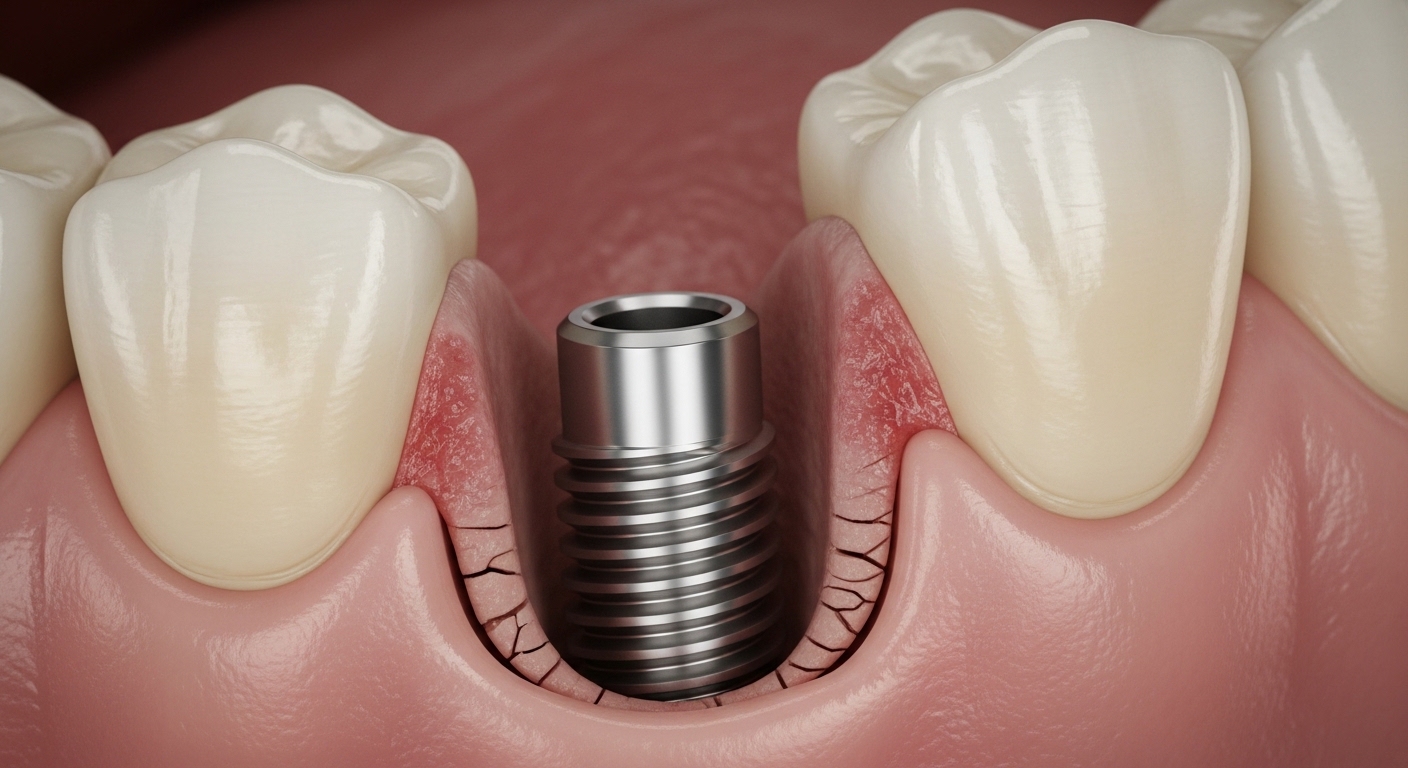
A dental implant is a biocompatible titanium artificial tooth root placed in the upper or lower jawbone. Its function is to support a dental prosthesis that replaces a missing tooth, restoring both chewing function and aesthetics.
Titanium is the most widely used material due to its ability to fuse with the bone in a process known as osseointegration.
Difference Between Risk, Complication, and Failure
- Risk: the possibility of an adverse event occurring
- Complication: a problem that arises but can be treated
- Failure: loss of the implant due to lack of integration or irreversible damage
This distinction is important: most risks do not lead to failure when properly managed.
Types of Dental Implant Risks
Immediate Surgical Risks
During implant placement, mild and manageable complications may occur:
- Temporary swelling or discomfort
- Minor bleeding
- Localized infection
Thanks to techniques such as computer-guided surgery, these risks are minimized by ensuring precise implant placement.
Risks During Osseointegration
Osseointegration is the phase in which the implant bonds with the bone. It is a critical biological process that typically lasts 2 to 4 months.
- Failure of bone integration
- Implant mobility
- Tissue inflammation
If this process fails, the implant cannot function properly and must be removed.
Medium- and Long-Term Risks: Peri-Implantitis
Peri-implantitis is the most significant long-term complication. It is an infection of the tissues surrounding the implant.
- Progressive bone loss
- Gum inflammation
- Possible implant loss
It affects a small percentage of patients, especially those who do not maintain proper oral hygiene.
Mechanical and Functional Risks
Implants can also be affected by mechanical factors:
- Fracture of the crown or prosthesis
- Loosening of screws
- Occlusal overload
These issues are often related to usage or habits such as bruxism (teeth grinding).
Factors That Increase Dental Implant Risk
Patient-Related Factors
- Uncontrolled diabetes
- Osteoporosis
- Systemic diseases
These conditions can affect healing and implant integration.
Clinical Factors
- Insufficient bone volume
- Pre-existing infections
- Periodontal disease
Poor bone support or active infections increase the risk of implant failure.
Habit-Related Factors
- Smoking: significantly increases the risk of implant failure
- Poor oral hygiene
- Bruxism: causes excessive pressure on the implant
These factors are modifiable and can be addressed before treatment.
How to Minimize Dental Implant Risks
Clinical Framework to Reduce Risks
- Comprehensive diagnostic evaluation
- Personalized digital treatment planning
- Use of advanced technology
- Minimally invasive surgery
- Ongoing follow-up and maintenance
The Importance of Diagnosis
A proper diagnosis allows evaluation of bone quality, detection of infections, and creation of a treatment plan tailored to each patient.
Technology in Implant Dentistry
- 3D imaging to assess bone structure
- Intraoral scanning for digital precision
- Guided surgery for maximum accuracy
These tools reduce errors and improve treatment safety.
Maintenance and Follow-Up
Long-term success depends largely on proper maintenance:
- Daily oral hygiene
- Regular check-ups
- Professional cleanings
Dental Implant Success Rate
Dental implants have one of the highest success rates in modern medicine. Compared to other solutions:
- Dental implants: >90–95% success rate
- Removable dentures: lower stability and durability
This confirms that, although risks exist, they are statistically low when treatment is performed to a high standard.
What Happens If a Dental Implant Fails?
In the event of failure:
- The implant is removed
- The affected area is cleaned
- Bone regeneration may be performed if needed
- A new implant can be placed later
Failure is not necessarily permanent—it is a manageable stage within the treatment process.
How to Detect Problems Early
Early detection of symptoms is key:
- Persistent pain
- Gum inflammation
- Bleeding when brushing
- Implant mobility
If any of these symptoms appear, it is essential to consult a specialist promptly.
Conclusion: Controlled Risks in Modern Implant Dentistry
Dental implant risks do exist, but they are predictable, manageable, and preventable. The key to success lies in three pillars:
- Accurate diagnosis
- Advanced technology
- Professional expertise
When these elements are combined, dental implants become a safe, durable, and high-quality solution for restoring your smile.
Frequently Asked Questions About Dental Implant Risks (FAQs)
Yes, they are one of the safest treatments when properly planned and executed.
Peri-implantitis, often associated with poor oral hygiene.
There is no true “rejection,” but in rare cases, the implant may fail to integrate with the bone.
Yes, it significantly increases the risk of implant failure.
Proper diagnosis, advanced technology, and regular follow-up care.